Understanding lymphedema
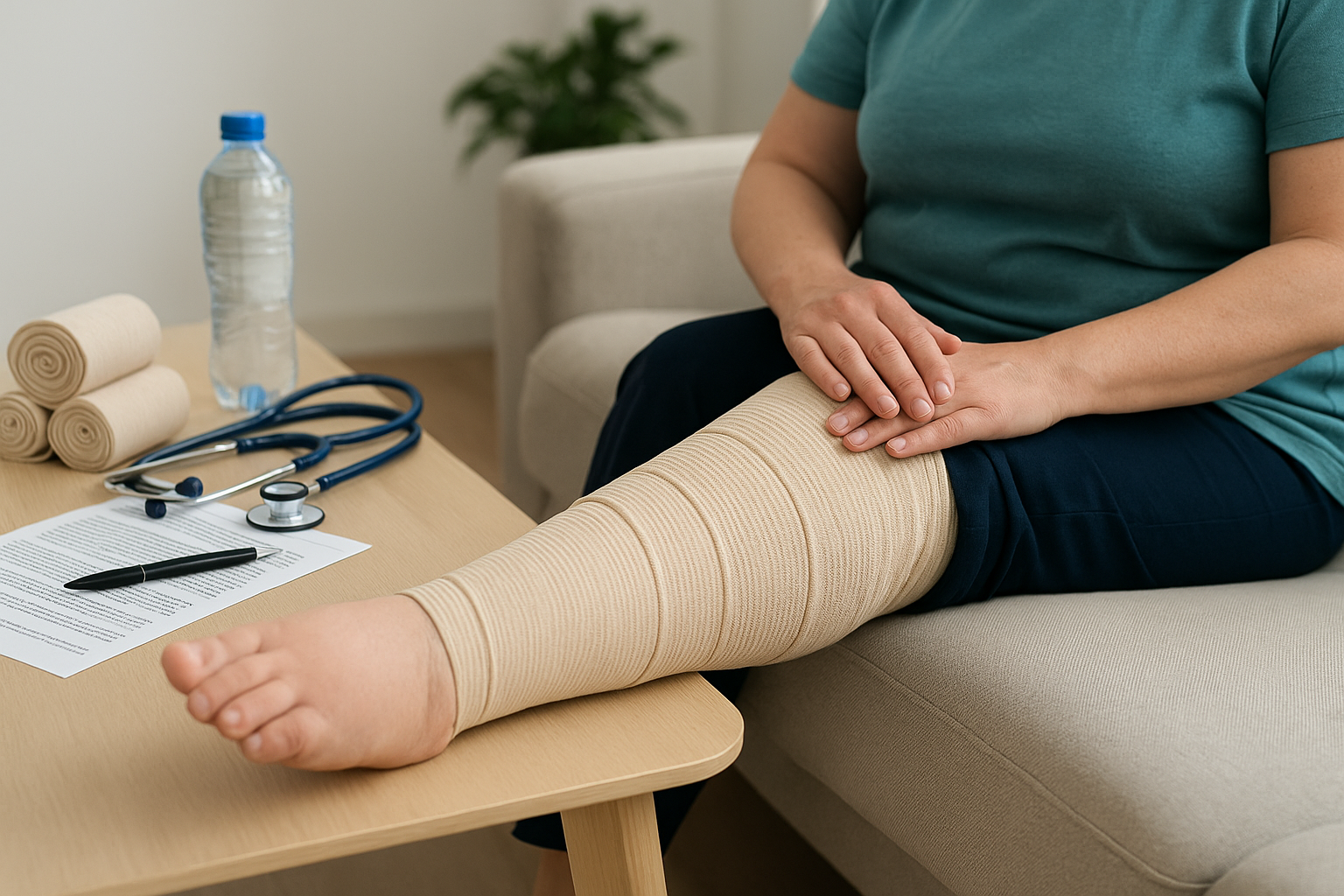
Lymphedema is swelling that happens when lymph fluid builds up in soft tissues because the lymphatic system can’t drain properly. It most often affects an arm or leg, but it can occur in other parts of the body. While there is no guaranteed cure for lymphedema, many proven techniques can significantly reduce swelling, improve comfort, and lower the risk of complications.
Daily self-care strategies
Consistent daily care is the foundation of controlling lymphedema. Small habits add up and keep swelling more stable over time.
Elevate and rest strategically
Elevating the affected limb above heart level for periods during the day helps gravity assist lymph drainage. Aim for short, frequent elevation sessions—10–20 minutes several times a day—rather than one long session. Balance rest with gentle movement to avoid stiffness.
Manage weight and hydration
Maintaining a healthy weight reduces pressure on lymphatic vessels. Focus on a balanced diet rich in vegetables, lean protein, and whole grains. Staying well-hydrated and moderating salt intake can also help minimize fluid retention.
Avoid constriction and injury
Loose clothing and non-restrictive jewelry help prevent extra pressure that can worsen swelling. Protect the affected limb from cuts, insect bites, sunburn, and other injuries—breaks in the skin can lead to infection and spikes in lymphedema.
Compression therapy
Compression is one of the most effective ways to reduce and manage lymphedema swelling.
Compression bandages vs. garments
Short-stretch compression bandaging is often used in intensive treatment phases to actively reduce volume. Once swelling is controlled, custom or off-the-shelf compression garments (sleeves, stockings) are worn daily to maintain results. Garments come in different compression levels—your therapist will recommend the right one.
How to get fitted and use garments
Proper fit is critical. A certified fitter or lymphedema therapist will measure your limb and recommend the correct size and compression class. Wear garments throughout the day and remove them at night unless otherwise advised by your clinician.
Manual lymphatic drainage (MLD) and massage
Manual lymphatic drainage is a specialized, gentle massage technique that helps move lymph fluid out of congested areas.
What to expect from professional MLD
A trained lymphedema therapist will use light, rhythmic strokes to stimulate lymph flow, often combined with compression bandaging as part of Complete Decongestive Therapy (CDT). CDT is the gold-standard intensive approach for reducing significant swelling.
Simple self-MLD basics
While self-MLD is not a replacement for professional care, you can learn gentle techniques to assist drainage between appointments: start with diaphragmatic breathing, then use light strokes from the center of the body outward toward healthy lymph nodes, always moving from congested areas toward drainage points.
Exercise and movement
Movement is medicine for lymphedema. Muscle contractions act like a pump to push lymph fluid through vessels.
Types of helpful exercises
- Low-impact activities: walking, swimming, and cycling are excellent because they combine movement with cardiovascular benefits.
- Resistance and range-of-motion exercises: light weights, resistance bands, and stretching help strengthen muscles and improve lymph flow.
- Breathing exercises: deep diaphragmatic breathing supports central lymphatic return.
How to start safely
Begin slowly and increase intensity in small steps. Wear your compression garment during exercise if recommended by your clinician. If you notice increased pain, redness, or a sudden rise in swelling, stop and consult your healthcare provider.
Skin care and infection prevention
Keeping the skin healthy is essential because infections (cellulitis) can rapidly worsen lymphedema.
Moisturize and protect
Use fragrance-free moisturizers to maintain skin barrier function. Clean and inspect your skin daily for cracks, blisters, or insect bites. Treat minor cuts promptly with antiseptic and a clean dressing.
Watch for signs of infection
Seek prompt medical attention for increasing warmth, redness, fever, or sudden worsening of swelling—these may be signs of cellulitis or another infection requiring antibiotics.
When to seek professional help
Work with a healthcare team experienced in lymphedema: physicians, certified lymphedema therapists, and specially trained nurses. They can tailor a plan that includes CDT, compression, garments, and exercise guidance.
Red flags
- Rapid, painful increase in swelling
- Fever, chills, or red streaks on the skin
- Open wounds that won’t heal
If any of these occur, contact your clinician or seek urgent care.
Conclusion
Reducing lymphedema swelling is a long-term, active process that combines compression, manual techniques, targeted exercise, careful skin care, and lifestyle adjustments. With consistent self-care and support from trained professionals, many people achieve meaningful improvements in swelling and quality of life. Talk with your healthcare team to create a plan that fits your needs and goals.