Understanding Debridement: What and Why
Debridement is the removal of devitalized tissue, foreign material, and biofilm from a wound to promote healing. It’s a fundamental step in managing acute and chronic wounds—diabetic foot ulcers, pressure injuries, venous leg ulcers, and surgical wounds all benefit when necrotic tissue is appropriately removed. Multiple debridement methods exist, each with advantages and limitations. This post compares sharp (surgical) debridement with other commonly used techniques to help clinicians and caregivers make informed choices.
Types of Debridement
Sharp (Surgical) Debridement
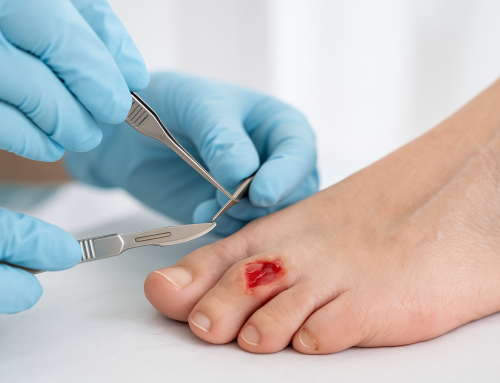
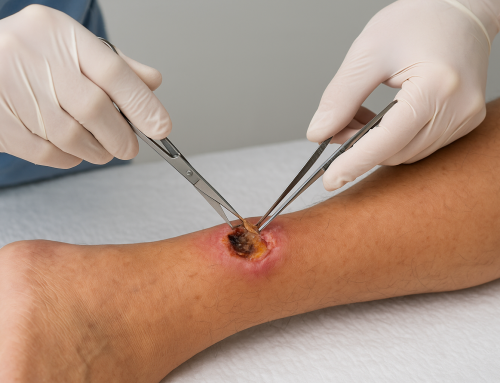
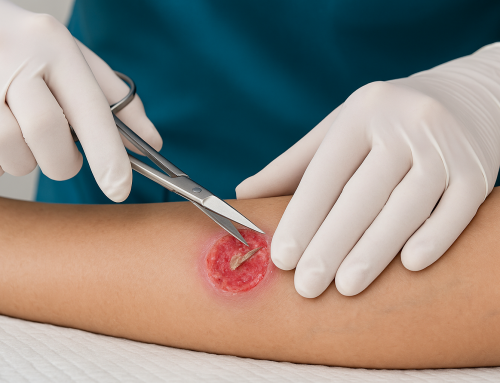
Sharp debridement uses scalpels, scissors, curettes, or other instruments to rapidly excise necrotic tissue and biofilm. It can be performed at bedside, in clinic, or in the operating room depending on wound complexity and patient factors. When done correctly, sharp debridement provides immediate reduction of bacterial load and devitalized tissue, often accelerating healing.
Mechanical Debridement
Mechanical methods include wet-to-dry dressings, wound irrigation, and wound scrubbing. These approaches physically remove debris but are less selective than sharp debridement and can damage viable tissue if not used carefully. They are inexpensive and accessible, making them common in many settings.
Autolytic Debridement
Autolytic debridement harnesses the body’s own enzymes and moisture to break down necrotic tissue. It’s achieved via occlusive or semi-occlusive dressings (e.g., hydrogels, films). This method is selective and painless but slower, making it suitable for stable wounds with minimal infection risk.
Enzymatic Debridement
Topical proteolytic enzymes (collagenase, bromelain-based products) chemically digest necrotic tissue. Enzymatic debridement is more rapid than autolytic methods and can be useful when sharp debridement is not feasible, but it requires ongoing application and monitoring for sensitivity reactions.
Biological (Maggot) Debridement
Sterile larvae of Lucilia sericata selectively consume necrotic tissue and secrete antimicrobial substances. Maggot therapy is highly selective and effective for stubborn, chronic wounds but may have limited acceptability and requires trained providers.
Hydrosurgical and Ultrasound-Assisted Debridement
These are newer technologies: hydrosurgery uses pressurized saline to excise tissue, while ultrasound-assisted devices disrupt biofilm and necrotic tissue. They can be precise and reduce thermal damage, often used when conventional sharp debridement has limitations.
Sharp Debridement vs Other Methods: Key Comparisons
Speed and Efficacy
Sharp debridement is typically the fastest way to remove large amounts of necrotic tissue and reduce bacterial burden. In infected or heavily necrotic wounds, it often delivers the most immediate clinical improvement. Autolytic and enzymatic methods are slower and better suited to less urgent or lower-volume necrosis.
Selectivity and Tissue Preservation
Autolytic, enzymatic, and biological methods are more selective for necrotic tissue, reducing risk to healthy tissue. Skilled sharp debridement can also be selective, but in inexperienced hands it risks removing viable tissue. New technologies (hydrosurgery, ultrasound) aim to combine speed with improved selectivity.
Pain, Bleeding, and Infection Risk
Sharp debridement can be painful and may cause bleeding; analgesia or local anesthesia is often necessary. It may also transiently increase bacterial dissemination if not paired with appropriate antimicrobial strategies. Noninvasive methods are generally less painful but may not adequately address infection or heavy biofilm.
Resource and Setting Considerations
Sharp debridement requires trained personnel and instruments; operating room debridement adds costs and anesthesia considerations. Mechanical and autolytic methods are low-cost and more accessible in resource-limited settings. Biological and advanced technological options require specialized supply chains or equipment.
Choosing the Right Method: Clinical Scenarios
Decision-making should be individualized. Consider sharp debridement when rapid tissue removal is needed—large devitalized areas, spreading infection, or ischemic tissue threatening limb viability. Use autolytic or enzymatic methods for medically fragile patients where surgery isn’t possible. Biological therapy suits chronic, nonhealing ulcers with thick slough. Combine approaches when appropriate—sharp debridement to reduce bulk followed by autolytic dressings to manage residual slough.
Practical Tips for Clinicians and Caregivers
- Assess vascular supply and infection status before debridement; revascularization may be needed for ischemic limbs.
- Use sharp debridement in controlled settings with appropriate analgesia and hemostasis techniques.
- Document wound bed, exudate, and pain before and after debridement for monitoring.
- Consider combination therapy: initial sharp debridement followed by enzymatic or autolytic dressings to optimize healing.
- Educate patients and caregivers about expected outcomes, dressing changes, and signs of infection.
Conclusion
No single debridement method fits every wound. Sharp debridement offers speed and immediate removal of necrotic tissue—often essential in infected or extensive wounds—while other methods provide selectivity, less pain, and suitability for patients who cannot tolerate sharp procedures. The best approach balances wound characteristics, patient factors, resources, and clinician expertise. Thoughtful selection and, when appropriate, combination of techniques will support faster healing and better outcomes.